Does Medicare Cover Transportation Checklist for Caregivers Calling Plans
Navigating Medicare transportation benefits can feel overwhelming when you're caring for a loved one who needs regular medical appointments. Medicare Part B covers 80% of medically necessary ambulance transportation after you meet the annual $283 deductible, but coverage for routine rides to doctor visits depends on whether your loved one has Original Medicare or a Medicare Advantage plan.
As a caregiver, knowing exactly what to ask and which documents to gather before calling a plan can save hours of frustration and ensure your loved one never misses a critical appointment. At Rosa Healthcare, we help families verify benefits and coordinate reliable medical transport, so you can focus on what matters most.
This guide provides a step-by-step checklist, call scripts, and resources you need to confirm transportation coverage quickly.

Do Medicare Plans Cover Transportation
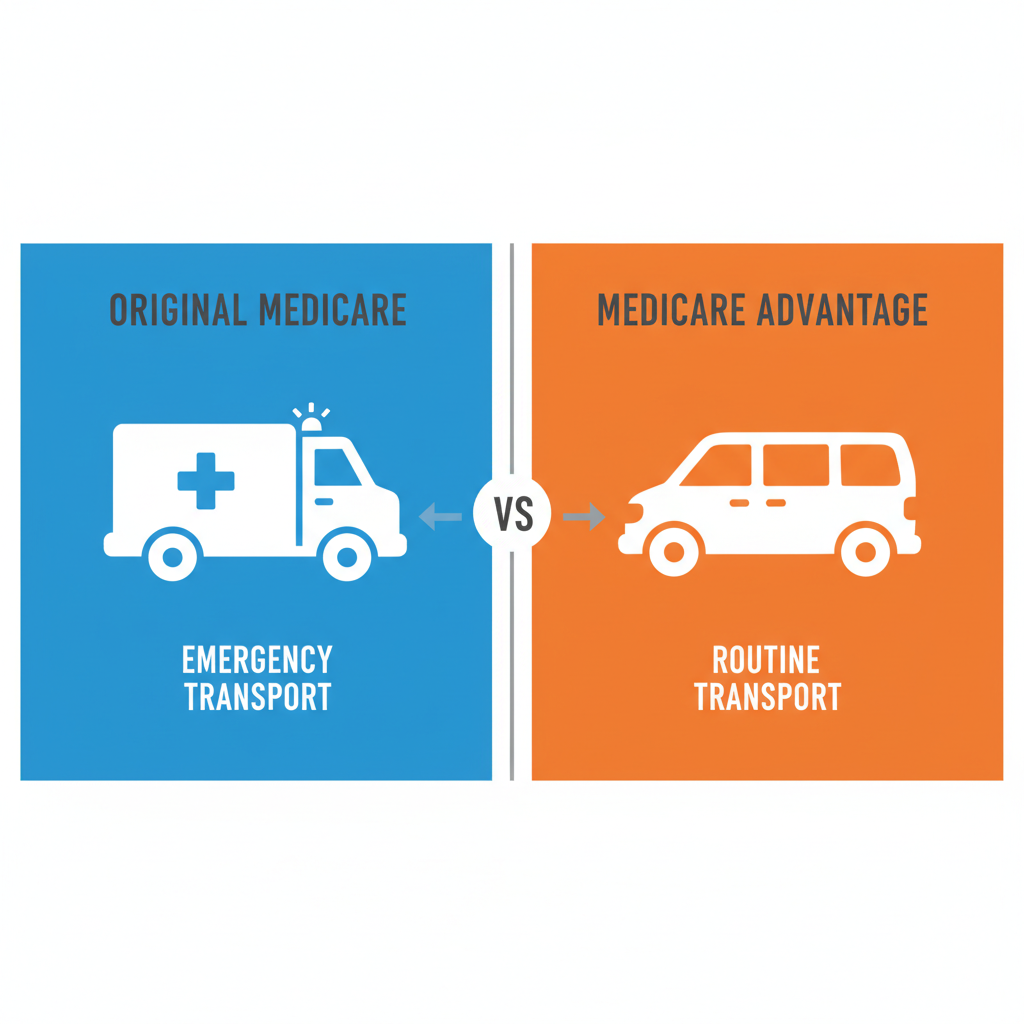
Understanding what Medicare covers for transportation starts with knowing which type of plan your loved one has. The coverage rules differ significantly between Original Medicare and Medicare Advantage plans.
Original Medicare offers limited transportation benefits. Medicare Part B covers emergency ambulance services when transportation is medically necessary to protect the patient's health. This includes ground ambulances to hospitals, skilled nursing facilities, or critical access hospitals. For non-emergency situations, Part B may cover ambulance rides only if a doctor provides a written order stating that other forms of transportation would endanger the patient's health. Common examples include dialysis patients with end-stage renal disease who need regular transport to treatment centers.
Medicare Advantage plans provide broader options. According to AARP, 36% of regular Medicare Advantage plans and 88% of Medicare Advantage Special Needs Plans offered transportation benefits for medical needs in 2024. These plans may cover up to 36 one-way trips per year to doctor appointments, pharmacies, therapy sessions, and other approved health-related locations at no copay. Some plans even extend benefits to fitness centers and wellness programs.
Key differences exist between the two coverage types. Original Medicare requires medical necessity documentation and typically covers only ambulance services. After meeting the Part B deductible of $283 in 2026, beneficiaries pay 20% coinsurance on approved rides. Medicare Advantage plans often include routine non-emergency medical transportation as a supplemental benefit, with trip limits varying by plan and region.
CMS rules create exceptions worth knowing. Medicare may cover air ambulance transport via helicopter or airplane when ground transportation cannot reach the patient quickly enough or the location is inaccessible. Coverage always extends only to the nearest appropriate medical facility capable of treating the patient's condition. If a beneficiary chooses a more distant hospital for personal preference, Medicare pays only what transport to the nearest facility would have cost.
Special Needs Plans offer enhanced benefits for chronically ill patients. Since 2020, Medicare Advantage plans can offer Special Supplemental Benefits for the Chronically Ill, which may include non-medical transportation to grocery stores, senior centers, and community events. According to KFF research, 6.1% of regular plans and 29.8% of special needs plans provided non-medical transportation in 2024.
Rosa Healthcare works directly with Medicare and Medicare Advantage plans to verify coverage and coordinate rides for patients who qualify. Our team understands the documentation requirements and can help families navigate prior authorization when needed.
Checklist for Caregivers to Verify Benefits

Before calling a Medicare or Medicare Advantage plan, gather all necessary information to make the verification process efficient. Use this comprehensive checklist to prepare.
Information to Collect Before You Call
Plan Identification Details:
- Medicare or Medicare Advantage plan name (e.g., UnitedHealthcare, Humana, Aetna)
- Member ID number (found on insurance card)
- Plan type (Original Medicare Part A/B, Medicare Advantage HMO, PPO, or Special Needs Plan)
- Group number if applicable
- Effective date of coverage
Patient Information:
- Full legal name as it appears on Medicare card
- Date of birth
- Current address and phone number
- Primary care physician name and contact information
Transportation Coverage Questions:
- Does the plan cover non-emergency medical transportation?
- How many one-way trips are included per year?
- What is the mileage limit per trip?
- Which destinations are approved (doctor offices, pharmacies, dialysis centers, therapy appointments)?
- Are wheelchair-accessible vehicles included?
- Can a companion ride along at no extra charge?
Prior Authorization Requirements:
- Is prior authorization required for transportation?
- How many days in advance must rides be scheduled?
- Who can request rides (member, caregiver, case manager)?
- What documentation is needed from the physician?
Cost and Billing Information:
- Is there a copay per trip?
- Does transportation count toward the plan deductible?
- Are costs different for in-network vs. out-of-network providers?
- What happens if all allocated trips are used?
Vendor and Scheduling Details:
- Which transportation vendor does the plan use?
- What is the vendor's phone number and scheduling portal?
- Can rides be booked online or only by phone?
- What is the cancellation policy?
- How long before the appointment should rides be scheduled?
Documentation to Keep on File
Create a transportation benefits folder with copies of:
- Evidence of Coverage (EOC) document highlighting transportation section
- Summary of Benefits showing trip limits and copays
- Transportation vendor contact card
- Confirmation numbers from scheduled rides
- Any written orders from physicians authorizing transportation
- Advance Beneficiary Notice forms if applicable
Red Flags to Watch For
Be alert to plan limitations that could cause problems:
- Network restrictions that require using specific transportation providers
- Geographic boundaries limiting where rides can go
- Time-of-day restrictions (some vendors operate only during business hours)
- Exclusions for certain appointment types
- Benefit resets that occur mid-year versus calendar year
Rosa Healthcare maintains current relationships with major Medicare Advantage plans and can help caregivers verify benefits before appointments are scheduled. Our care coordinators know which questions to ask and can advocate on your behalf.
Sample Call Script for Plan Benefit Verification
Having a prepared script keeps your call focused and ensures you get all the information you need in one conversation. These templates work for phone calls and online chat support.
Phone Call Script
Opening:
"Hello, my name is [Your Name], and I'm calling to verify transportation benefits for my [relationship: mother, father, spouse]. I'm their primary caregiver and have their permission to discuss their coverage. The member's name is [Patient Full Name], date of birth [DOB], and member ID is [ID Number]."
Core Questions:
"I'd like to confirm a few details about non-emergency medical transportation benefits:
- Does this plan include transportation to medical appointments? If yes, how many one-way trips are covered per year?
- What types of destinations are approved? Can we use rides for doctor appointments, physical therapy, dialysis, and pharmacy visits?
- Is there a mileage limit per trip, and what is the maximum distance covered?
- Do we need prior authorization, and how far in advance should rides be scheduled?
- Which transportation vendor should we contact to book rides, and what is their phone number?
- Is there a copay or any out-of-pocket cost per trip?
- Are wheelchair-accessible vehicles available if needed?
- Can I, as the caregiver, schedule rides on their behalf, or does the member need to call directly?"
Confirmation and Follow-Up:
"Thank you. Can I please have your name and a reference number for this call? Could you also email or mail written confirmation of these benefits to [your email/address]? Is there anything else I should know about using this benefit?"
Closing:
"I appreciate your help. If I have questions after scheduling a ride, what's the best number to call back?"
Online Chat Script
Opening Message:
"Hello, I need to verify non-emergency medical transportation benefits. Member Name: [Full Name], DOB: [Date], Member ID: [Number]. I am the authorized caregiver."
Question List:
"Please confirm:
- Number of covered one-way trips per year
- Approved destinations (doctor, pharmacy, therapy, etc.)
- Mileage limit per trip
- Prior authorization requirements
- Transportation vendor name and contact
- Copay amount per trip
- Wheelchair vehicle availability
- Whether caregiver can schedule rides
Can you send a summary of this coverage to my email [address]?"
Follow-Up Message:
Thankyou for providing your services!!
"Thank you. Please provide a reference or case number for my records and confirm the vendor phone number to schedule rides."
What to Do If Coverage Is Denied or Unclear
If the representative cannot confirm transportation benefits:
- Ask to speak with a supervisor or benefits specialist
- Request a callback from the transportation vendor directly
- Ask for the specific policy section in your Evidence of Coverage document
- Inquire about alternative benefits such as mileage reimbursement programs
- Document the date, time, representative name, and reason for denial
If your loved one qualifies for both Medicare and Medicaid (dual eligibility), Medicaid may cover non-emergency medical transportation that Medicare does not. Ask the representative to check coordination of benefits.
Rosa Healthcare can step in when caregivers encounter barriers with insurance verification. Our team regularly works with plan representatives and knows how to escalate coverage questions efficiently.
How Rosa Can Help Check Benefits and Book Rides
Navigating insurance benefits and coordinating reliable transportation should not add stress to caregiving. Rosa Healthcare offers comprehensive support that removes the burden from families.
What We Do
Rosa Healthcare provides RN-supervised medical transportation and home healthcare services tailored to individual patient needs. We handle benefit verification, prior authorization, and ride scheduling so caregivers can focus on their loved ones. Our team has established relationships with major Medicare Advantage plans and understands exactly what documentation is required.
When you contact us, we immediately verify your loved one's transportation benefits at no charge. We check trip limits, copays, vendor requirements, and any restrictions. If prior authorization is needed, we coordinate directly with the physician's office to obtain the necessary medical orders.
Our Transportation Services Include
24/7 Medical Transport: Our vehicles are equipped to safely transport patients with mobility limitations, wheelchairs, and medical equipment. Drivers receive specialized training in patient assistance and gentle care techniques.
Ambulatory Assistance: We provide door-through-door service, helping patients from their home to the vehicle and into the medical facility. No patient is left to navigate stairs, curbs, or long walks alone.
Appointment Coordination: We schedule rides in alignment with medical appointments, therapy sessions, dialysis treatments, and other recurring healthcare needs. Reminder calls ensure patients are ready when transportation arrives.
Compassionate Patient Support: Every member of our team understands the dignity and respect elderly and disabled patients deserve. We move at the patient's pace and accommodate individual comfort needs.
Why Families Choose Rosa Healthcare
Reliability matters when health is at stake. Rosa Healthcare maintains on-time arrival rates above industry standards because we know missed appointments can lead to declined health. Our dispatch system tracks every ride in real time and communicates any delays immediately.
We accept Medicare Advantage transportation benefits from most major plans and work with families to minimize out-of-pocket costs. If a plan does not cover transportation or trips are exhausted, we offer affordable private-pay rates.
Our intake process is simple. Call our office or visit our website to provide the patient's insurance information. Within 24 hours, we confirm coverage and can schedule the first ride. For recurring appointments, we set up a standing schedule so transportation is automatic.
Getting Started
Contact Rosa Healthcare to verify your loved one's transportation benefits and book their first ride. Our care coordinators are available to answer questions about coverage, scheduling, and our services. Whether your loved one needs a single ride to a specialist or daily transport for dialysis, we provide the gentle, reliable care they deserve.
Visit Rosa Healthcare or call our office to speak with a coordinator today. We are here to help families access the medical care they need without the stress of navigating insurance and logistics alone.
Key Takeaways
- Original Medicare covers ambulance services for emergencies and medically necessary situations with a doctor's order, but not routine rides to appointments.
- Medicare Advantage plans may offer up to 36 one-way trips per year for medical appointments, with coverage varying by plan and region.
- Caregivers should gather plan details, member ID, and physician information before calling to verify transportation benefits.
- Use structured call scripts to ask about trip limits, mileage caps, prior authorization, approved destinations, and vendor contact information.
- Rosa Healthcare verifies benefits at no charge and coordinates reliable, compassionate medical transportation for Medicare and Medicare Advantage members.
Frequently Asked Questions
Does Original Medicare cover rides to doctor appointments?
Original Medicare covers ambulance services only when medically necessary. Routine rides require a doctor's written order stating other transportation would endanger health.
How many rides does Medicare Advantage cover per year?
Most Medicare Advantage plans offering transportation benefits cover 24 to 48 one-way trips annually. Exact limits vary by plan and location.
Can caregivers schedule rides on behalf of patients?
Yes, most plans allow authorized caregivers, legal guardians, or case managers to schedule transportation on the member's behalf after verifying identity.
What happens if I run out of covered trips?
Contact your plan's member services to explore options. Some plans offer additional trips for chronically ill members or alternative benefits like mileage reimbursement.
Does Rosa Healthcare accept Medicare transportation benefits?
Yes, Rosa Healthcare works with most major Medicare Advantage plans that include transportation benefits. We verify coverage and handle billing directly with insurers.

Leave a Reply